10 ways physiotherapy can help improve your overall health

Physiotherapists provide assistance to persons who have been hurt, are unwell, or have a disability through movement and exercise, manual treatment, education, and counselling. By shielding people of all ages from illness, they help patients manage their discomfort and maintain their health.
Physical therapy’s role in daily life is important:
It is untrue that a physiotherapist can only assist patients at home who have been dealing with acute or chronic difficulties; physiotherapy may also assist people in building up their bodies, remaining active, maintaining excellent posture, and maintaining appropriate ergonomics at work.
Physiotherapists work with individuals of all ages to alleviate constraints on physical function. Working with patients before and after surgery, assisting individuals who are recuperating from an illness or chronic disease, an injury, a vehicle or industrial accident, or assisting those with age-related illnesses are some examples of this.
Because our home physiotherapists have extensive clinical experience and are obviously passionate about what they do, their patients are more likely to continue working, participating in society, and enjoying life. Physical therapists are essential in helping people achieve their goals at every stage of life.
If you're still unsure as to why physical therapy is such an important field, consider these ten advantages:
- To alleviate or eliminate discomfort through natural healing. Stretching and physical treatment are frequently used to treat pain.
- Preventing surgery and/or caring for patients through pre- and post-surgical rehab. Improving mobility through a variety of stretches and range-of-motion exercises.
- Recover from a stroke: Balance, muscular strength, range of motion, sensitivity, coordination, and endurance are among the elements that physiotherapists focus on since they are crucial for mobility.
- By putting the person through rigorous sports training, decrease or avoid sports injuries.
- Improve your balance to prevent falls, especially if you’re elderly and your balance is impaired by ailments such as Parkinson’s disease or old age.
- Promoting lifestyle adjustment and embracing a healthy lifestyle to manage diabetes and vascular diseases by obtaining enough sleep, maintaining a nutritious diet, engaging in physical activity and keeping a healthy weight.
- Elderly care: The patient is taught by the physiotherapist how to adjust to sight, movement, balance, and muscle loss deficits so that they may easily carry out activities of daily life. This awareness lowers the possibility of injuries and re-injuries.
- Aiding in the treatment of lung and heart conditions with a cardiac rehabilitation course that include chest rehabilitation and deep breathing exercises. Additionally, they have been demonstrated to reduce the heart rate, drop or stabilise blood pressure, and lessen stress.
- Health of Women: All conditions affecting the pelvis and pelvic floor are therapeutically treated with physiotherapy. For a woman to remain fit and healthy throughout her life, even throughout pregnancy, after giving birth, and after surgery, exercise is essential.
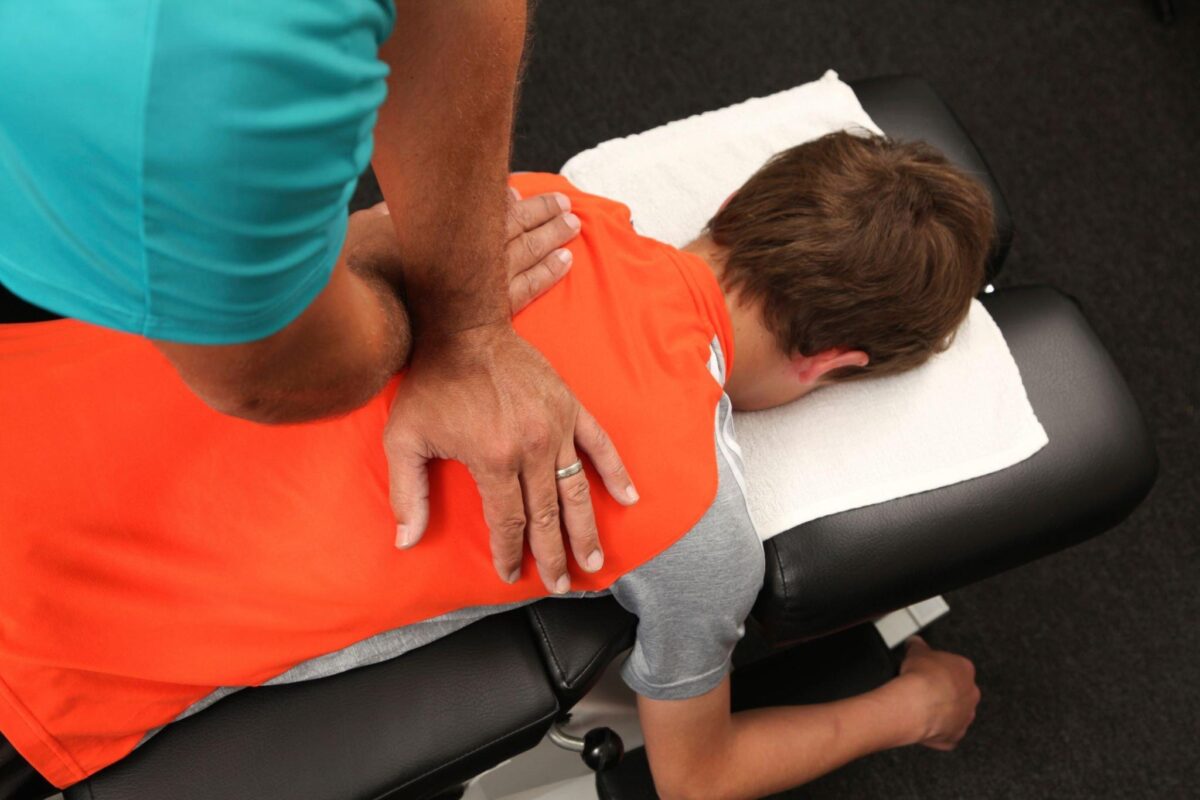
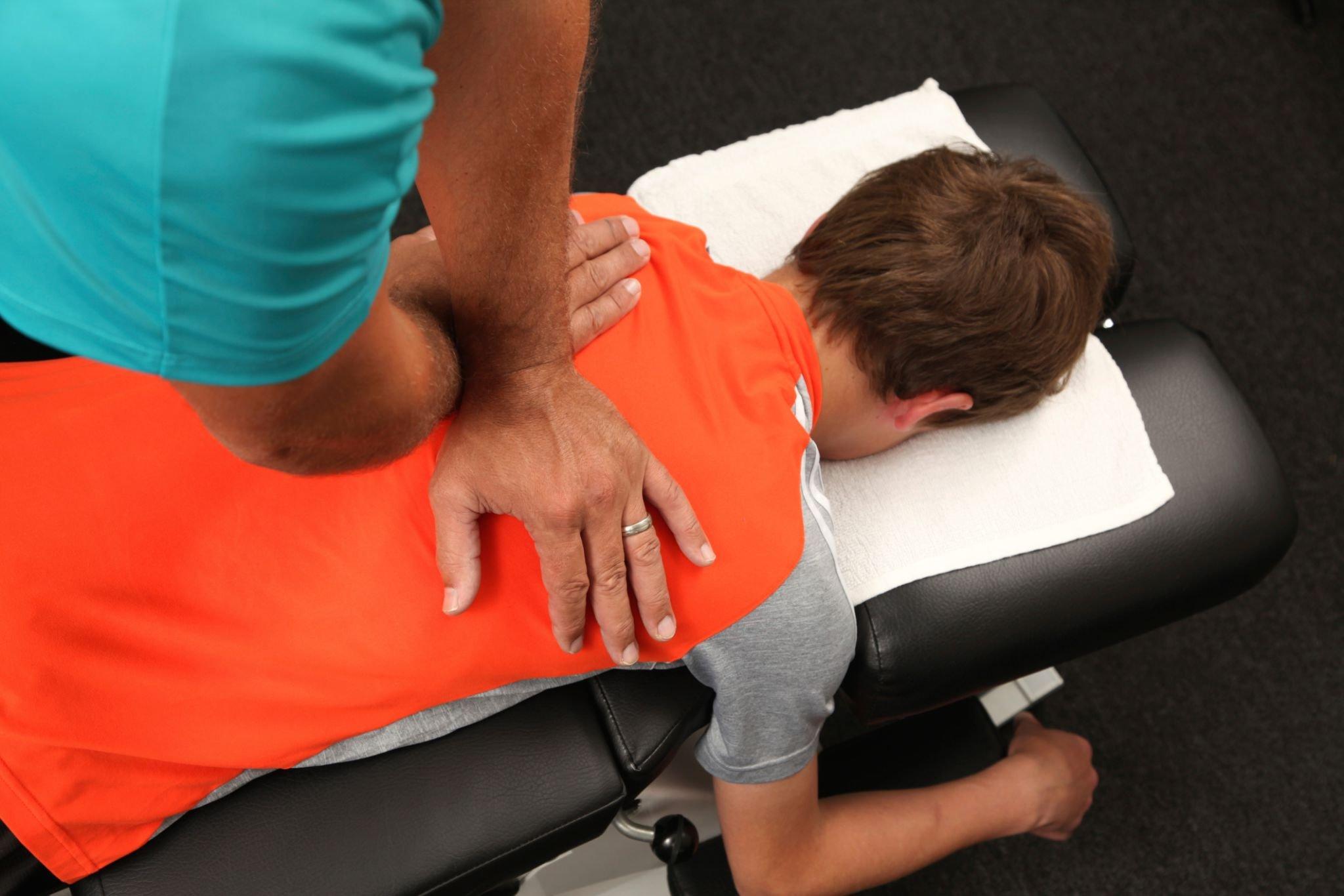
- Paediatric Physiotherapy: The paediatric practitioners are well-versed in the relationship between regular child development and the systems and processes of the body. While paediatric physiotherapists employ many of the general physiotherapy techniques, they also use additional abilities and education in the area of growth and development to treat babies through adolescence.
The following are the primary points to emphasise the importance of therapy:
- Staying active increases, a person’s likelihood of continuing to work, socialise, and enjoy life on their own.
- If you want to retain your health, keep moving throughout your life.
- Millions of deaths each year are directly related to inactivity, which also makes people more disabled. It could increase the risk of diseases like diabetes, heart disease, and stroke. Cancer, diabetes, heart disease, and stroke are among the illnesses that could get worse as a result.
- Any age can reap the rewards of exercise, and even just 30 minutes per day of moderate activity, such brisk walking, can have a significant impact.
Physiotherapists support a quick recovery in addition to encouraging behaviours and lifestyle changes that could improve general health and well-being. You can only achieve fitness and rehabilitation through frequent therapy and the use of the best medical procedures and supplies by remaining in touch with your physiotherapist at the proper time. Don’t be late; schedule an appointment with our expert physiotherapist in or WhatsApp at 8929020020. Stay tuned for additional blog updates.